Synopsis
Your body needs the right amount of blood flow to keep your heart pumping, your legs moving and your brain functioning. Blood circulation, the movement of blood throughout the body, is clearly crucial to your existence, and poor leg circulation can cause many problems for individuals around the world.
A common cause of poor leg circulation – restricted blood flow to your legs – is peripheral vascular disease, or PVD. This term refers to disorders involving blood vessels outside, or on the periphery, of the heart. PVD can involve peripheral arteries (blood vessels that carry blood away from the heart) or peripheral veins (blood vessels that carry blood toward the heart).
When PVD involves the arteries, it is known as peripheral artery disease, or PAD. A fatty substance called plaque builds up and hardens on the walls of the peripheral arteries, making it difficult for blood to properly flow through. The plaque takes years to build up, which is why older adults are more at risk.
In addition, the following behaviors or conditions can also contribute to foot, ankle and lower leg circulation problems:
- Tobacco smoking
- Obesity
- Lack of exercise
- Improper diet
- High blood pressure
- High cholesterol
- Diabetes
- Certain nerve and thyroid conditions
- Pregnancy
- Long periods of sitting in a cramped and immobile position (Economy Class Syndrome)
Symptoms:
If you have poor leg circulation, symptoms usually develop gradually.
- In the early stages, you may experience cramping or fatigue in the legs, buttocks or feet during activity. The pain, whether it’s leg pain, lower leg pain or foot pain, usually diminishes with rest, but will reoccur.
- You may complain of a tired, aching feet, or swollen feet/legs.
- You may also have cramping that occurs in your legs and feet when you are sleeping or immobile for extended periods of time.
- In addition, you can incur such symptoms as ‘cold feet,’ or feet that ‘fall asleep.’
Frequent suffering with cold feet and/or cold hands usually signifies that your circulation, or blood flow from your heart, has slowed. This may especially happen at night when you are trying to sleep, during periods of immobility or after eating certain foods.
People who have very poor leg circulation may also develop a blood clot, a sudden blockage in blood that can cause severe leg pain. This blood clot, known as deep vein thrombosis (DVT), develops in a deep vein, and can occur when a vein is damaged or if blood flow slows down or stops completely. If you’re obese and/or over age 40, you’re at particular risk for DVT.
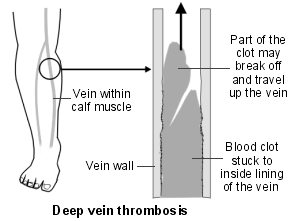
When a blood clot forms in a leg vein it usually remains stuck to the vein wall. The symptoms tend to settle gradually. But, there are two main possible complications:
- Pulmonary embolus (a blood clot which travels to the lung).
- Post thrombotic syndrome (persistent calf symptoms).
Pulmonary embolus
In a small number of people who have a DVT, a part of the blood clot 'breaks
off'. This travels in the bloodstream and is called an embolus. An embolus will
travel in the bloodstream until it becomes stuck. An embolus that comes from a
clot in a leg vein will be carried up the larger leg veins to the heart, through
the large heart chambers, but will get stuck in a blood vessel going to a lung.
This is called a pulmonary embolus. A small pulmonary embolus may not cause any
symptoms. A medium sized pulmonary embolus can cause breathing problems and
chest pain. A large pulmonary embolus can cause collapse and sudden death.
Post-thrombotic syndrome
Without treatment, up to 6 in 10 people who have a DVT develop long-term
symptoms in the calf. This is called 'post-thrombotic syndrome'. Symptoms occur
because the increased flow and pressure of the diverted blood in other veins can
affect the tissues of the calf. Symptoms can range from mild to severe and
include: calf pain, discomfort, swelling, and rashes. An ulcer on the skin of
the calf may develop in severe cases. Post-thrombotic syndrome is more likely to
occur if the DVT occurs in a thigh vein, or extends up into a thigh vein from a
calf vein.
Phlegmasia Alba Dolens (Blue Leg)
Progression of the clotting process in the vein may lead to increased swelling. This can cause a global compromise of the circulation in the limb, affecting both the arteries and the veins. This complication is called phlegmasia alba dolens and may lead to gangrene, requiring amputation of the affected limb.
Treatment and Prevention
The aims of treatment are:
- To prevent the clot spreading up the vein and getting larger. This prevents the possibility of a large embolus breaking off and travelling to the lungs.
- To reduce the risk of post-thrombotic syndrome developing.
- To prevent a further DVT in the future.
Anticoagulation - preventing the
clot from getting bigger
Anticoagulation is often called 'thinning the blood'. However, it does not
actually thin the blood. It alters certain chemicals in the blood to stop clots
forming so easily. This prevents a DVT from getting bigger, and prevents any new
clots from forming. Warfarin is the usual anticoagulant. However, it takes a few
days for warfarin tablets to work fully. So, heparin injections are often used
in the first few days for immediate effect. A serious embolus is rare if you
start anticoagulation treatment early after a DVT.
The aim is to get the dose of warfarin just right so the blood will not clot easily, but not too much which may cause bleeding problems. You will need regular blood tests whilst you take warfarin. You need them quite often at first, but then less frequently once the correct dose is found. (If you are pregnant, regular heparin injections rather than warfarin tablets may be used.)
Compression and raising the leg -
to prevent post-thrombotic syndrome
If the DVT was in a thigh vein, you may be advised to wear a compression
stocking. With this treatment the risk of developing post-thrombotic syndrome is
much reduced. You should wear the stocking each day, for at least 2 years.
(Symptoms of post-thrombotic syndrome may develop even several months after a
DVT, which is why you should wear the stocking long-term.)
The slight pressure from the stocking helps to prevent fluid seeping into the calf tissues from the outer veins which carry the extra diverted blood following a DVT. The stocking also reduces, and may prevent, calf swelling. This in turn reduces discomfort and the risk of skin ulcers forming.
If you are advised to wear a compression stocking, you should put it on each day whilst lying in bed before getting up. Wear it for the whole day until you go to bed, or until you rest in the evening with the leg raised. Take the stocking off before going to bed.
In addition, the following are also commonly advised.
- Raise your leg when you are resting. This too reduces the pressure in the calf veins, and helps to prevent blood and fluid from 'pooling' in the calves. 'Raised' means that your foot is higher than your hip so gravity helps with blood flow returning from the calf. The easiest way to raise your leg is to recline on a sofa with your leg up on a cushion.
- Raise the foot of the bed a few inches if it is comfortable to sleep like this. This is so your foot and calf are slightly higher than your hip when you are asleep.
Preventing a first DVT - or a
recurrence of a DVT
A DVT is often a 'one-off' event after a major operation. In this situation you
will normally be advised to stop taking warfarin after a few months. Some people
have an ongoing risk of a further DVT. For example, if you have a blood clotting
problem, or continued immobility. You may then be advised to continue taking
warfarin long-term.
Other things that may help to prevent a first or recurrent DVT include the following.
- If possible, avoid long periods of immobility such as sitting in a chair for many hours. If you are able, get up and walk around now and then. A daily brisk walk for 30-60 minutes is even better if you can do this. The aim is to stop the blood 'pooling', and to get the circulation in the legs moving. Regular exercise of the calf muscles also helps. You can do some calf exercises even when you are sitting.
- Major surgical operations are known to be a risk for a DVT - particularly operations to the hip, lower abdomen, and leg. You may be given aspirin or heparin just before having an operation to help prevent a DVT. An inflatable sleeve connected to a pump to compress the legs during a long operation may also be used. It is also common practice to get you up and walking as soon as possible after an operation.
- When you travel on long plane journeys, train journeys, etc, you should have little walks up and down the aisle every now and then. Also, exercise your calf muscles every now and then whilst sitting in your seat.
See your physician if you suspect you have poor leg circulation, as the condition can be serious and an indication of another medical problem. Medications are available to treat leg circulation problems and to help prevent more serious consequences.