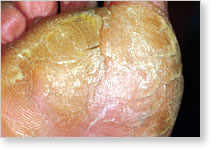
Diabetic Foot Neuropathy
Synopsis
The
patient with diabetes is at risk of losing feeling in the feet. This is the
result of changes in glucose metabolism that affect the ability of the nerve to
conduct electrical impulses. There are two types of neuropathy. One is the lack
of feeling and sensation, which leads to skin and bone problems. The other,
referred to as autonomic neuropathy, is associated with changes in the skin
texture and the moisture and oiliness of the skin. The combination of autonomic
and sensory neuropathy leads to dry skin with scaling, fissuring and cracks,
particularly on the bottom of the foot.
 |
Note the thickened skin on the bottom of the foot. This can lead to cracks and an infection in the foot. The thick-scaled skin is aggravated by the condition of neuropathy. |
Treatment of
neuropathy begins with good care of the feet. The feet should be inspected for
sores and pressure areas twice daily. A mirror is often helpful. Socks should be
changed frequently and there should be no pressure areas between the sock and
the shoe. The shoe should be well padded and fitted by a shoe specialist (a
pedorthist). A soft insole, called an orthotic support, should be used to
protect and pad the foot from pressure. The condition of the skin must be
maintained by soaking the feet regularly in room temperature water. Soak the
foot daily for about 10 minutes and then rub in Vaseline to keep the skin soft
and pliable. This will prevent cracks and fissures from forming. It does not
appear that any medications or surgery can improve the condition of neuropathy.